This post is also available in: Persian Armenian
If we were to choose a single element as the symbol of aerobic life, oxygen would undoubtedly top the list. About 21% of Earth’s atmosphere consists of oxygen, and this element has played a fundamental role in shaping biological evolution. The introduction of oxygen into Earth’s atmosphere around 2.4 billion years ago—during an event known as the “Great Oxidation Event”—fundamentally altered the course of life’s evolution. Organisms that could harness oxygen for energy production gained a significant evolutionary advantage due to the higher efficiency of aerobic metabolism compared to anaerobic pathways.
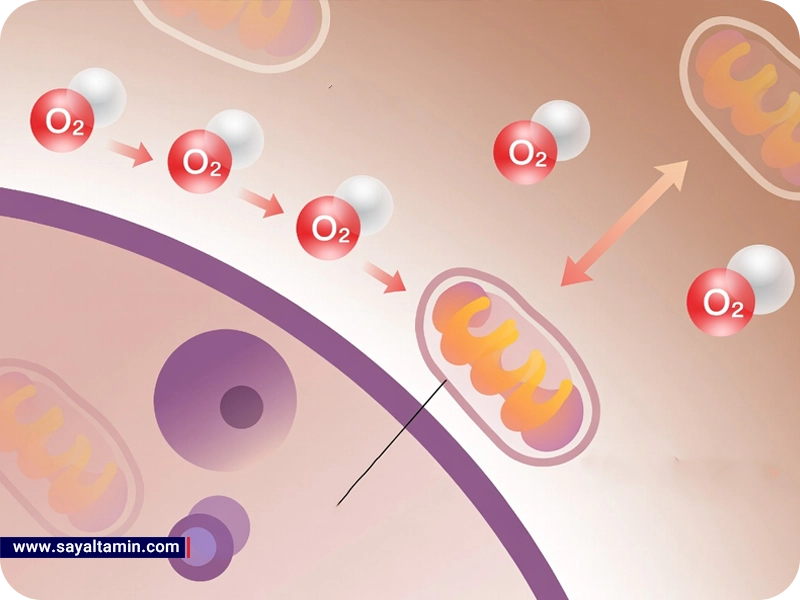
In humans, nearly every cell depends on oxygen for survival. Interrupting oxygen supply for even a few minutes can lead to cell death and irreversible tissue damage, particularly in high-energy-demand tissues such as the brain and heart. Yet, the very oxygen essential for survival can, at the molecular level, become a destructive agent.
This biological paradox—oxygen as both a source of life and a potential cause of damage—is one of the most fascinating topics in cellular and molecular biology. Understanding this duality is crucial not only for medicine and biotechnology but also for industrial sectors involved in oxygen production, storage, and transport, since oxygen quality, purity, and control can profoundly affect living systems.
Oxygen and Cellular Metabolism: The Engine of Life
1. Cellular Respiration: From Glucose to ATP
To understand oxygen’s role in metabolism, we must first examine the cell’s energy production pathways. Cellular respiration is a multi-step process in which the chemical energy stored in organic molecules (such as glucose) is converted into ATP. This process includes three main stages:
- Glycolysis (in the cytosol)
- Krebs cycle or citric acid cycle (in the mitochondrial matrix)
- Electron transport chain and oxidative phosphorylation (in the inner mitochondrial membrane)
During the first two stages, high-energy electrons are extracted from fuel molecules and transferred to carriers such as NADH and FADH₂. However, the decisive step for bulk ATP production is the electron transport chain, where oxygen plays a central role.
2. Oxygen as the Final Electron Acceptor
In the electron transport chain, electrons are passed through a series of membrane-bound protein complexes. At the end of this chain, oxygen serves as the final electron acceptor, combining with electrons and protons to form water:
O₂ + 4e⁻ + 4H⁺ → 2H₂O
This seemingly simple reaction is, in fact, vital for cell survival. Without oxygen, the electron transport chain halts, and ATP production drops sharply. Under such conditions, cells resort to anaerobic pathways, such as fermentation, which are far less energy-efficient.
Approximately, complete aerobic metabolism of one glucose molecule can generate around 30–32 ATP molecules, whereas anaerobic conditions yield only about 2 ATP. This stark difference highlights oxygen’s critical importance in human physiology.
3. Mitochondria: Powerhouse and Potential Source of Damage
Mitochondria are often referred to as the “cellular powerhouse,” but in addition to energy production, they are a major source of reactive oxygen species (ROS). Under normal conditions, about 1–2% of the oxygen consumed in the electron transport chain is not fully reduced to water and instead forms partially reduced species, such as superoxide (O₂•⁻).
Under physiological conditions, this small amount of ROS is not harmful and even plays a role in regulating cellular signaling. However, if ROS production increases or cellular defense systems weaken, the delicate balance between production and neutralization is disrupted, leading to oxidative stress.
Oxygen’s Second Face: From Biological Signal to Oxidative Stress
Molecular oxygen (O₂) in its ground state is relatively stable. However, its unique electronic configuration—specifically, two unpaired electrons in separate orbitals—makes it readily participate in redox reactions under certain conditions. This property allows energy extraction from biological fuels while also enabling the formation of reactive and potentially damaging derivatives.
Within the cell, oxygen is never simply an inert gas; it participates in a complex network of electron exchanges. In this dynamic environment, some oxygen is not fully reduced to water and forms partially reduced species known as reactive oxygen species (ROS).
ROS: An Inevitable Consequence of Aerobic Metabolism
ROS production is not a biological error. Rather, it is a natural and unavoidable outcome of using oxygen as the terminal electron acceptor. In mitochondria, where the electron transport chain operates to generate ATP, electrons pass through protein complexes. While highly efficient, this process is not perfectly complete.
A small fraction of electrons reacts with oxygen before reaching the chain’s end, producing superoxide. Although this may seem minor—perhaps only 1–2% of total oxygen consumed—consider that each human cell consumes billions of oxygen molecules daily, turning this small fraction into a substantial number of reactive molecules.
Superoxide can convert into hydrogen peroxide, and in the presence of metal ions like iron, can generate hydroxyl radicals—among the most chemically damaging biological species. This cascade illustrates the intrinsic risks of aerobic metabolism.
Regulatory Role of ROS: Rethinking an Old Notion
For years, ROS were viewed solely as harmful metabolic byproducts. However, research over the past two decades has revealed that cells use ROS as signaling molecules.
Contrary to popular belief, hydrogen peroxide is not merely a destructive oxidant; it can reversibly oxidize thiol groups in proteins, modulating their activity. Many signaling pathways—including those governing growth, differentiation, stress response, and even energy metabolism—are sensitive to subtle ROS fluctuations.
Cells have effectively learned to use “controlled danger” as a regulatory tool, a phenomenon sometimes referred to as redox signaling, where the balance of oxidation and reduction becomes part of the cell’s communication language. Yet, as with any signaling system, precision is critical—the line between beneficial and harmful effects is narrow.
When Balance Collapses: Oxidative Stress
In healthy cells, ROS production and neutralization are dynamically balanced. Enzymatic and non-enzymatic antioxidant systems constantly suppress reactive species. However, if this balance is disrupted—due to increased energy demand, chronic inflammation, environmental toxins, mitochondrial dysfunction, or weakened defense systems—oxidative stress occurs.
Oxidative stress is not merely an increase in ROS numbers; it reflects the biological system’s inability to manage their consequences. In this state, essential cellular molecules become targets for oxidative reactions.
Membrane lipids rich in unsaturated fatty acids are highly vulnerable to radical attack. Lipid peroxidation can alter membrane structure and fluidity, disrupt ion channels, and even trigger cell death signals. In lipid-dense tissues like the brain, such damage is particularly significant.
Proteins are also susceptible. Oxidation can disrupt their three-dimensional structure, impairing function. Damaged proteins may aggregate into insoluble structures, a phenomenon observed in neurodegenerative diseases like Alzheimer’s.
Perhaps most critically, ROS target genetic material.
DNA: Memory Under Oxidative Attack
DNA, both nuclear and mitochondrial, is continuously exposed to oxidative insults. Chemical modifications of nitrogenous bases, single- and double-strand breaks, and point mutations are among the consequences.
While cells possess DNA repair systems, these mechanisms are not perfect. Over time, some damage accumulates. This gradual buildup forms the basis of theories that link molecular damage to aging.
Mitochondrial DNA (mtDNA) is particularly vulnerable. Small and circular, mtDNA is located near ROS production sites and lacks the extensive histone protection of nuclear DNA. Damage to mtDNA can impair electron transport chain efficiency, further increasing ROS production. This negative feedback loop is one proposed mechanism explaining age-related decline in cellular function.
Table 2 – Functional Spectrum of ROS: From Regulation to Damage
| ROS Level | Physiological State | Biological Outcome |
|---|---|---|
| Very low | Normal signaling | Growth and differentiation regulation |
| Moderate, controlled | Stable redox balance | Normal metabolic function |
| High, persistent | Oxidative stress | Lipid and protein damage |
| Very high | Cellular collapse | Apoptosis or necrosis |
Oxygen, Inflammation, and Systemic Aging
A more complex aspect is that ROS can activate inflammatory pathways. Chronic, low-level activation of inflammatory factors produces a condition some researchers call inflammaging.
This state triggers a continuous cycle of immune system activation. Persistent, mild inflammation can contribute to age-related diseases, including cardiovascular disease, type 2 diabetes, and neurological disorders.
Thus, oxygen influences not only cellular but also systemic aging processes.
Oxygen, Oxidative Stress, and Biological Theories of Aging
Aging: Genetically Programmed or Damage Accumulation?
Aging is a multidimensional phenomenon with no definitive answer. Is it the result of a predetermined genetic program, or the cumulative effect of molecular damage over time? Among various theories, one of the most influential is the free radical theory of aging, directly linked to oxygen’s dual role.
In the 1950s, Denham Harman proposed that continuous production of free radicals during aerobic metabolism gradually damages cellular components, and the accumulation of these damages forms the biological basis of aging. This theory was revolutionary, as it was the first to directly link energy metabolism with aging processes.
According to this view, the more an organism uses oxygen, the more free radicals are produced, accelerating the accumulation of damage. Simply put, the “cost of respiration” is the cost of life.
Yet, biological science never stops evolving.
Revisiting the Free Radical Theory
In recent decades, experimental data have become more complex than what the original simplistic theory could accommodate. Some organisms with high metabolic rates live surprisingly long. Certain animal models with elevated antioxidant levels did not exhibit significant lifespan extension. In some cases, even mild increases in ROS were associated with increased longevity.
These findings revealed that ROS are not merely “random toxins” but integral components of life’s regulatory network. Consequently, the classical free radical theory evolved into more modern versions emphasizing “disruption of redox balance” and “adaptive stress signaling.”
A key concept emerging from this revision is known as hormesis.
Hormesis: When Mild Stress Becomes Beneficial
Hormesis refers to a phenomenon in which exposure to low levels of a stressor activates defensive pathways and ultimately enhances cellular resilience. In the context of oxygen, mild and controlled increases in ROS can trigger protective mechanisms.
Examples include:
- Activation of the transcription factor Nrf2, increasing the expression of antioxidant genes
- Stimulation of DNA repair pathways
- Enhancement of mitochondrial efficiency
Thus, low ROS levels can act as an “alert signal,” strengthening cellular defense systems. However, chronic or excessive stress can overwhelm these defenses, resulting in dominant cellular damage.
This perspective demonstrates that the relationship between oxygen and aging is not linear or straightforward—it depends on intensity, duration, and the biological context.
Mitochondria at the Center of the Aging Equation
Almost all modern aging models place mitochondria at the core. This is logical: mitochondria are both the primary energy source and a major ROS producer.
With aging, key mitochondrial changes are observed:
- Decline in electron transport chain efficiency
- Increase in electron leakage
- Accumulation of mutations in mitochondrial DNA (mtDNA)
- Reduced ATP production capacity
These changes can form a vicious cycle: mitochondrial dysfunction → increased ROS → further damage → greater dysfunction.
However, some studies show that mild mitochondrial ROS increases early in life can activate longevity pathways. This suggests that the quality of oxidative signaling is more critical than the mere quantity of ROS.
Calorie Restriction: Reducing or Optimizing Oxygen Use?
One of the most robust interventions in animal models for lifespan extension is calorie restriction without malnutrition. Studied since the 1930s, this intervention has extended lifespan across species—from yeast to mammals.
Initial hypotheses suggested that calorie restriction reduces metabolism and oxygen consumption, thereby lowering ROS production. More detailed studies, however, revealed a more complex picture.
Calorie restriction activates specific molecular pathways, including:
- Sirtuins (especially SIRT1)
- AMPK
- mTOR inhibition
These pathways improve mitochondrial efficiency, increase autophagy (clearing damaged components), and strengthen cellular resilience. In effect, calorie restriction not only modulates oxygen consumption but optimizes its utilization.
In other words, the central question may not be “how much oxygen do we consume?” but rather “how do we use it?”
Table 3 – Molecular Pathways, ROS, and Aging
| Molecular Pathway | ROS Relationship | Effect on Aging |
|---|---|---|
| Nrf2 | Activated by mild ROS | Upregulates antioxidant genes |
| SIRT1 | Energy-dependent | Enhances DNA repair and mitochondrial efficiency |
| AMPK | Energy sensor | Stimulates efficient metabolism |
| mTOR | Nutrient-sensitive | Inhibition linked to lifespan extension |
| p53 | DNA damage response | Regulates cell death and cellular aging |
Cellular Senescence and Oxygen
Another critical aspect of oxygen-aging interplay is cellular senescence. In this state, cells exit the division cycle due to cumulative damage—including oxidative damage—but remain viable. These cells often secrete a set of inflammatory molecules that alter the tissue environment.
Accumulation of senescent cells in tissues is a hallmark of aging. Chronic oxidative stress is one of the primary triggers driving cells into this state.
Antioxidant Systems and Redox Balance Maintenance
How cells live with oxygen without being destroyed
If oxygen is considered a controlled flame that powers life, antioxidant systems act as the engineering mechanisms preventing that flame from becoming a wildfire. Aerobic life would be impossible without these protective systems. In fact, multicellular evolution occurred alongside mechanisms to manage energy derived from oxidation.
Cells constantly experience redox reactions in mitochondria, cytosol, nucleus, endoplasmic reticulum, and plasma membrane. Maintaining redox balance is therefore a dynamic, localized, and moment-to-moment process, not a static state.
First Line of Defense: Antioxidant Enzymes
At the heart of the cellular defense system are enzymes specifically designed to neutralize ROS. They are strategically localized and have rapid reaction kinetics.
- Superoxide dismutase (SOD): Converts superoxide to hydrogen peroxide, which is more stable and controllable. Cells possess multiple SOD isoforms: cytosolic, mitochondrial, and extracellular.
- Hydrogen peroxide is further degraded by catalase and glutathione peroxidase. Catalase converts it directly to water and oxygen, while glutathione peroxidase uses glutathione to reduce it to water.
This cascade demonstrates that the body does not merely remove ROS but manages them in a controlled, stepwise manner.
Glutathione: Pillar of Redox Balance
Among intracellular antioxidants, glutathione is particularly important. This small tripeptide exists in reduced (GSH) and oxidized (GSSG) forms. The ratio of GSH to GSSG is a key indicator of cellular redox status. When ROS increase, GSH is consumed. If the cell cannot regenerate it, redox balance shifts toward oxidative stress.
With aging, glutathione levels decline in many tissues, contributing to increased vulnerability to oxidative damage in the elderly.
Why Antioxidant Supplements Are Not Always Miraculous
For decades, it was thought that consuming antioxidant supplements like vitamin C, vitamin E, or beta-carotene could slow aging. Large clinical trials, however, revealed a more complex picture.
High-dose antioxidant supplementation often did not extend lifespan and, in some cases, increased the risk of certain diseases.
The explanation lies in hormesis: if ROS serve signaling roles at low levels, excessive elimination can disrupt adaptive pathways. The body requires a certain level of oxidative activity to maintain redox homeostasis. Complete suppression is neither possible nor desirable.
Redox Homeostasis: The Central Concept in Aging
Redox homeostasis refers to the dynamic balance between oxidation and reduction reactions in the cell, functioning like a biological thermostat. Neither excessive oxidation nor excessive reduction is optimal.
With aging, this biological thermostat falters: mitochondrial efficiency declines, repair systems weaken, glutathione levels drop, and inflammatory responses rise. The result is a gradual shift toward chronic oxidative states.
Oxygen remains essential for life, but the system’s ability to manage its consequences diminishes—explaining why age-related diseases are often accompanied by elevated oxidative stress markers.
Oxidative Stress, Oxygen, and Age-Related Diseases
When redox imbalance affects tissues and the whole organism
So far, oxygen has been examined at the cellular level: in mitochondria, DNA, signaling networks, and defense systems. Yet the consequences of redox imbalance extend beyond a single cell. With aging, cumulative changes across trillions of cells manifest in tissues and organs, transforming oxidative stress into a systemic phenomenon.
Chronic ROS accumulation combined with declining defense capacity creates an environment conducive to many age-related diseases. These conditions do not arise from “too much oxygen” per se, but from the inability of biological systems to handle its continuous consumption.
Cardiovascular Disease: Oxidation in Vessel Walls
A well-known example of oxidative stress involvement is atherosclerosis. Low-density lipoproteins (LDL) in vessel walls undergo oxidation. Oxidized LDL is recognized and engulfed by immune cells, eventually forming plaques in the vessel wall.
ROS play a key role in this process—they mediate LDL oxidation and activate inflammatory pathways. The ultimate consequence is reduced vascular flexibility, arterial narrowing, and increased risk of heart attack or stroke.
Endothelial cells (lining vessels) are also affected by oxidative stress with age. Nitric oxide production—critical for vessel dilation—declines, disrupting blood pressure regulation. Through these oxidative intermediates, oxygen becomes a major challenge to cardiovascular health in the elderly.
Type 2 Diabetes: A Vicious Cycle of Metabolism and ROS
In type 2 diabetes, insulin resistance and impaired glucose metabolism are accompanied by increased ROS production. Elevated blood glucose enhances electron flow in the electron transport chain, exacerbating electron leakage and superoxide generation.
ROS, in turn, amplify inflammatory pathways and impair insulin signaling, creating a vicious cycle: hyperglycemia → increased ROS → aggravated insulin resistance → further hyperglycemia.
Over time, oxidative stress in diabetes damages microvasculature, kidneys, retina, and peripheral nerves. Oxygen’s role in this disease is therefore evident not only at the cellular level but also in systemic complications.
Neurodegenerative Diseases: The Brain Against Oxidation
The brain is among the most sensitive tissues to oxidative stress. Oxygen consumption in neural tissue is extremely high, while neurons have limited capacity for division. Consequently, cumulative damage can have irreversible effects.
In Alzheimer’s disease, elevated markers of lipid and protein oxidation have been reported in brain tissue. In Parkinson’s disease, mitochondrial dysfunction and increased ROS are observed. The accumulation of abnormal proteins in these conditions can be both a cause and a consequence of oxidative stress.
Oxygen in the brain is as vital as it is demanding of precise management. Even minor disruptions in redox balance can impact memory, cognition, and neural function.
Cancer: A More Complex Duality
In cancer, the relationship with ROS is more complex. On one hand, oxidative damage to DNA can cause mutations that initiate tumorigenesis. On the other hand, many cancer cells maintain higher ROS levels and paradoxically use them to stimulate proliferation.
These cells simultaneously bolster their antioxidant systems to prevent death from excessive stress. This delicate balance has emerged as a potential target in anti-cancer therapies: disrupting redox homeostasis in cancer cells to drive them toward collapse.
Oxygen Therapy: The Boundary Between Benefit and Risk
In clinical settings, oxygen is a vital intervention—from intensive care units to treatment of pulmonary diseases and even hyperbaric medicine. Here, too, the principle of balance applies.
Excessive oxygen administration can cause oxygen toxicity, characterized by sharply elevated ROS that may damage lung tissue. Therefore, modern medicine emphasizes precise targeting of oxygen saturation, rather than simply increasing levels.
This underscores that oxygen must be used carefully, in a controlled manner, and proportionally to biological need, whether in humans or industrial applications where oxygen purity and supply are critical.
After examining oxygen’s role in metabolism, ROS production, aging, and age-related diseases, the key question arises: Is this process inevitable? Is aging merely the price of oxygen consumption, or can the biological response to it be modulated?
Current science offers an answer that is neither fully deterministic nor wholly optimistic. What is clear is that the human body is not a static system; it is a dynamic, adaptive network capable of increasing or decreasing its capacity to manage oxidative stress.
Exercise: Temporary ROS Increase to Strengthen Defense Systems
At first glance, it may seem counterintuitive, but exercise, which typically increases oxygen consumption, can improve redox balance. During physical activity, oxygen use in muscles rises, increasing ROS production. However, if this increase remains within physiological limits, it acts as a hormetic stimulus.
Regular training activates pathways such as Nrf2 and enhances the expression of antioxidant enzymes. The body responds to mild stress from exercise by boosting its defensive capacity. This explains why physically active individuals generally exhibit lower oxidative and inflammatory markers.
This example demonstrates again that oxygen and ROS are not inherently harmful; rather, their intensity and exposure pattern determine their effects.
Nutrition: Fuel Type and Redox Status Regulation
Metabolic fuel quality also influences ROS production. Diets high in simple sugars and processed fats can increase oxidative load, whereas diets rich in polyphenols, fiber, and beneficial fatty acids improve mitochondrial function.
Compounds such as resveratrol, curcumin, and flavonoids not only have direct antioxidant properties but also activate longevity-related signaling pathways. As noted previously, the goal is not to eliminate ROS entirely, but to support the body’s intrinsic regulatory systems.
Sleep and Circadian Rhythm
An emerging area in aging research is the role of the circadian rhythm in metabolism and redox regulation. Sleep disturbances are associated with increased oxidative stress markers. Regular sleep–wake cycles coordinate mitochondrial activity, DNA repair, and clearance of damaged molecules.
Emerging Technologies in Oxidative Stress Monitoring
Advances in biotechnology now allow measurement of oxidative markers in blood, urine, and tissues. Molecules such as 8-oxo-dG, malondialdehyde, and isoprostanes serve as indicators of oxidative damage.
In the future, integrating biological, genetic, and metabolic data may enable personalized redox profiling—an approach that could facilitate targeted interventions to maintain health during aging.
Industrial–Biological Perspective on Oxygen
For organizations involved in the production, storage, and supply of oxygen, understanding this biological complexity is crucial. Oxygen is not merely an industrial gas; it is a vital component in biomedicine, intensive care, biotechnology, and the food industry.
Control over oxygen purity, pressure, dosage, and delivery in therapeutic applications can directly impact tissue redox balance. Thus, engineering quality in industrial gas production indirectly intersects with cellular health.
Molecular Pathways Through Which Oxygen Influences Aging
From a molecular biology perspective, aging is not merely the result of simple cellular wear and tear. It arises from a complex interplay among metabolic signals, cellular energy status, oxygen levels, redox balance, and gene regulatory networks. Oxygen sits at the center of this network.
1. Free Radical Theory and Its Evolution
In the 1950s, Denham Harman proposed the Free Radical Theory of Aging, suggesting that free radicals generated during aerobic metabolism gradually damage vital cellular molecules, and that this cumulative damage is a primary cause of aging.
Today, we recognize that this theory requires refinement. The issue is not merely the presence of ROS but the imbalance between their production and removal. Specifically:
- Low levels of ROS act as signaling molecules.
- High levels of ROS are destructive.
This shift in thinking led scientists to focus not on total ROS elimination but on redox homeostasis.
Redox homeostasis is the maintenance of balance between oxidant species and cellular antioxidant systems. When this balance shifts toward oxidants, oxidative stress occurs—a hallmark of biological aging.
2. Oxidative Damage to DNA and Its Connection to Aging
DNA, the blueprint of life, is a major ROS target. Species such as hydroxyl radicals can:
- Oxidize nucleotide bases (e.g., forming 8-oxo-dG)
- Cause single- or double-strand DNA breaks
- Impair replication system efficiency
Although cells possess advanced DNA repair mechanisms (e.g., BER, NER, and HR), their efficiency declines with age.
3. Mitochondria: Both Source and Target of Damage
Mitochondria, as the main site of oxygen consumption, are naturally exposed to the highest ROS levels.
Unlike nuclear DNA, mitochondrial DNA (mtDNA):
- Lacks protective histones
- Has limited repair capacity
- Resides near the ROS source
4. Oxygen and the mTOR Pathway
One of the key regulators of lifespan is the mTOR (mammalian Target of Rapamycin) pathway.
mTOR senses energy status, nutrients, and growth signals. When nutrients are abundant, energy is sufficient, and cell growth is active, mTOR is activated, promoting cell division and protein synthesis.
Chronic mTOR activation, however, is associated with aging and age-related diseases, including cancer, diabetes, and neurodegenerative disorders.
Oxygen can influence mTOR activity through ATP production and redox status, while high ROS levels can modify downstream regulatory pathways. Notably, mTOR inhibition (e.g., by rapamycin) extends lifespan in animal models.
5. AMPK Pathway and Response to Metabolic Stress
Opposing mTOR, AMPK is activated when:
- ATP levels drop
- AMP/ATP ratio increases
- Cells experience energy stress
Oxygen indirectly regulates AMPK via ATP production. Under hypoxia, altered cellular energy status activates protective pathways.
6. HIF-1α: Oxygen Sensor at the Gene Level
HIF-1α is a major regulator of oxygen response.
- Under normal oxygen, HIF-1α is rapidly degraded.
- Under low oxygen, HIF-1α stabilizes, translocates to the nucleus, and induces genes involved in cell survival, angiogenesis, and glycolysis.
Dysregulation of this pathway contributes to aging and cancer. Interestingly, short-term controlled hypoxia can induce beneficial adaptive responses (hormesis).
7. Oxidative Hormesis: When Stress Becomes Beneficial
Hormesis describes a phenomenon in which a low level of a stressor elicits a beneficial adaptive response.
————————————————–
resource
Harman, D. (1956). Aging: A theory based on free radical and radiation chemistry. Journal of Gerontology.
López-Otín, C., Blasco, M.A., Partridge, L., Serrano, M., Kroemer, G. (2013). The hallmarks of aging. Cell.
Finkel, T., & Holbrook, N.J. (2000). Oxidants, oxidative stress and the biology of ageing. Nature.
Balaban, R.S., Nemoto, S., & Finkel, T. (2005). Mitochondria, oxidants, and aging. Cell.
Sena, L.A., & Chandel, N.S. (2012). Physiological roles of mitochondrial reactive oxygen species. Molecular Cell.
Ristow, M., & Schmeisser, S. (2014). Mitohormesis: Promoting health and lifespan by increased levels of reactive oxygen species (ROS). Dose-Response.